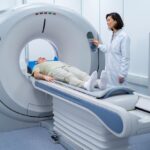
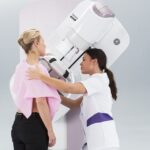
With the world’s population growing older, the number of elderly patients diagnosed with cancer is increasing at a rapid pace. Almost 60% of all cancers and more than 70% of cancer deaths occur in individuals 65 and older. Yet elderly cancer patients frequently have special challenges that are quite different from those of younger patients, necessitating an extremely individualized method of diagnosis, treatment, and recovery.
The Special Challenges of Geriatric Oncology
Older adults’ cancer is confounded by age-related physiological alterations, existing disease (comorbidities), diminished functional reserve, and social restrictions. Chemotherapy, surgery, or radiation can pose greater risk for the elderly patient, so judicious assessment is necessary.
For instance, older adults can have decreased kidney or liver function, which influences drug metabolism. They can also have more severe side effects from conventional treatments or have difficulty maintaining nutritional equilibrium during treatment. In other instances, the presence of multiple drugs (polypharmacy) poses a risk of adverse drug interactions.
Individualized Assessment: Not Just About Age
Age by itself cannot be the only consideration in designing a cancer treatment plan. Oncologists, rather, employ a comprehensive geriatric assessment (CGA) to assess a patient’s overall health status. It encompasses physical condition, cognitive status, emotional state, mobility, social support, and nutritional status.
The CGA assists physicians in determining whether the patient can withstand aggressive treatment or would be better served by a less intense strategy aimed at quality of life. It aids in the identification of reversible conditions such as malnutrition or depression that would improve prognosis.
Personalized Treatment Strategies
1. Surgery
Surgery can be therapeutic but is high-risk for frail older patients with compromised heart, lung, or kidney function. Minimally invasive procedures, including laparoscopic surgery, are being explored in elderly patients because they reduce recovery time and complications.
2. Chemotherapy
Older patients are at greater risk of chemotherapy-associated toxicities like fatigue, nausea, and infection. Oncologists may choose lower-dose regimens or less toxic oral chemotherapy drugs that are better tolerated. Supportive care in the form of growth factors or anti-nausea medication is crucial to prevent toxicity.
3. Radiation Therapy
Contemporary methods such as intensity-modulated radiation therapy (IMRT) and image-guided radiation therapy (IGRT) permit more accurate tumor targeting with less damage to healthy tissue. This is particularly advantageous for older patients, decreasing side effects and recovery time.
4. Targeted Therapy & Immunotherapy
More recent therapies such as targeted therapy and immunotherapy provide hopeful alternatives for older adults. These treatments have fewer systemic side effects than conventional chemotherapy and are specific to the genetic makeup of the cancer, which makes them more effective in certain situations.
Emphasis on Quality of Life
In older patients, independence and quality of life are usually a priority. Treatment objectives can then change from trying to cure to emphasizing comfort and quality of life, with emphasis placed on symptom control.Pain relief, fatigue management, emotional support, and physical therapy become essential elements of treatment.
The introduction of hospice and palliative care services early on in the course of treatment is able to help patients and families make decisions, control symptoms, and prepare for future care needs.
The Role of Caregivers and Family
Older patients largely depend on caregivers or family members for transportation, medication management, and psychologic support. The incorporation of caregivers in the process of treatment planning will help in setting realistic expectations, monitoring properly, and ensuring regular follow-up during therapy.
Caregiver burden must be evaluated by healthcare providers and resources must be given accordingly to avoid burnout.
Looking Ahead: The Need for Geriatric Oncology Specialists
As cancer treatment continues to progress, there is an urgent demand for oncologists with expertise in treating geriatric patients. These professionals are able to balance aggressive cancer therapies with the sensitive needs of older bodies. In most nations, cancer facilities are now incorporating geriatric oncology departments, providing multidisciplinary care involving oncologists, geriatricians, nurses, dietitians, and social workers.
Conclusion
Elderly cancer is an increasing fact of life that calls for understanding, sensitive evaluation, and individualized treatment. By centering attention not solely on the illness but on the individual as a whole, oncology staff are able to administer successful treatment without compromising the patient’s dignity, wishes, and way of life. With the evolution of medical technology and increased sensitivity to geriatric issues, elderly cancer treatment is constantly enhancing — bringing hope, alleviation, and restoration to the golden years.
Summay
Cancer care in the aged demands a sensitive, individualized strategy because of age-related health issues. With almost 60% of cancer incidence developing in patients over 65, customized care comes into play. New cancer treatments such as targeted therapy, minimally invasive surgery, and precision radiation therapy provide safer and better options for the elderly. With the able direction of Dr. Jagdish Shinde, Pune and PCMC’s eminent oncologist, geriatric patients are afforded individualized care in harmony with treatment objectives—palliative or curative—as well as comfort and quality of life. Through early palliative care intervention and supportive caregiver care, elderly patients can tolerate treatment with dignity. Dr. Shinde makes sure that all patients access state-of-the-art cancer therapy as per their individual requirements.